Contents
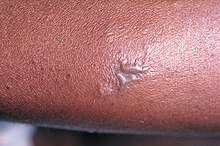
Gonococcemia (also known as "Disseminated gonococcal infection"[1]) is a rare complication of mucosal Neisseria gonorrhoeae infection, or Gonorrhea, that occurs when the bacteria invade the bloodstream.[2] It is characterized by fever, tender hemorrhagic pustules on the extremities or the trunk, migratory polyarthritis, and tenosynovitis.[3] It also rarely leads to endocarditis and meningitis.[4] This condition occurs in 0.5-3% of individuals with gonorrhea, and it usually presents 2–3 weeks after acquiring the infection.[5] Risk factors include female sex, sexual promiscuity, and infection with resistant strains of Neisseria gonorrhoeae. This condition is treated with cephalosporin and fluoroquinolone antibiotics.[4]
Epidemiology
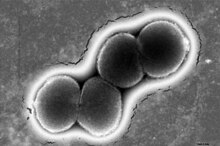
Neisseria gonorrhoeae is a gram negative diplococcus (also referred to as "Gonococcus") and a pathogenic bacteria.[2] In 2019, there were 616,392 reported cases of gonorrhea in the United States, with an overall increased rate 5.7% from 2018 to 2019.[6] Among those approximately 600,000 cases, it is estimated that 0.5-3% of gonorrheal infections result in gonococcemia. This condition is more common in women, affecting approximately 2.3-3% of women with gonorrhea and 0.4-0.7% of men.[4] This discrepancy is explained by increased incidence of silent gonorrheal infections in females and an increased rate of transmission to females that have sexual intercourse with infected males.[5] Gonococcemia also occurs more frequently in pregnant women, those with recent menstruation, and those with IUDs.[5]
Risk Factors
- Infection with certain strains of Neisseria gonorrhoeae[3]
- Prolonged infection[3]
- Female sex (due to asymptomatic infection, and therefore prolonged infection)[3]
- Sexual promiscuity[3]
- Immune system deficiencies[3]
- Infection during menstruation, pregnancy, or in the puerperium period[3]
Symptoms
- Fever
- Migratory arthralgias
- Hemorrhagic pustules
- Tenosynovitis
- Rarely headache, neck stiffness, and visual changes (associated with meningitis)
Treatment
Treatment typically consists of cephalosporin and fluoroquinolone antibiotics.[4] Gonococcemia is typically treated with intravenous or intramuscular cephalosporin antibiotics.[5] Approximately 10-30% of gonorrheal infections present with a co-infection of chlamydia, so it is common to add a one-time dose of oral azithromycin or doxycycline for coverage of Chlamydia trachomatis.[5] Bacterial resistance to antibiotics is increasingly common in Neisseria gonorrhoeae, so it is often advised to check susceptibility of the bacterial culture and then adjust the antibiotic therapy as needed.[4]
Pathogenesis
Neisseria gonorrhoeae is transmitted during sexual contact with an infected individual. The bacteria invade the non-ciliated columnar epithelium of the urogenital tract, oral mucosa, or anal mucosa following exposure.[2] Invasion of the host cells is made possible due to virulence factors such as Pili, LOS, Opa, and others.[2] Similarly, these virulence factors can be used for avoiding the host immune system, which may explain prolonged infection, bacterial resistance, and gonococcemia.[3]
See also
References
- ^ a b Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.[page needed]
- ^ a b c d Hill, Stuart A.; Masters, Thao L.; Wachter, Jenny (2016). "Gonorrhea - an evolving disease of the new millennium". Microbial Cell. 3 (9): 371–389. doi:10.15698/mic2016.09.524. ISSN 2311-2638. PMC 5354566. PMID 28357376.
- ^ a b c d e f g h Shirtliff, Mark E.; Mader, Jon T. (October 2002). "Acute Septic Arthritis". Clinical Microbiology Reviews. 15 (4): 527–544. doi:10.1128/CMR.15.4.527-544.2002. ISSN 0893-8512. PMC 126863. PMID 12364368.
- ^ a b c d e Creighton, Sarah (2014-02-21). "Gonorrhoea". BMJ Clinical Evidence. 2014: 1604. ISSN 1752-8526. PMC 3931440. PMID 24559849.
- ^ a b c d e Beatrous, Surget V.; Grisoli, Stratton B.; Riahi, Ryan R.; Matherne, Ryan J.; Matherne, Ryan J. (2017). "Cutaneous manifestations of disseminated gonococcemia". Dermatology Online Journal. 23 (1). doi:10.5070/D3231033674. PMID 28329470.
- ^ "National Overview - Sexually Transmitted Disease Surveillance, 2019". www.cdc.gov. 2021-04-19. Retrieved 2021-11-03.

